💊 medicine
Blood Transfusion and Massive Blood Transfusion Protocol Complete Clinical Guide
Comprehensive clinical guide on blood transfusion and massive blood transfusion protocol covering indications, components, transfusion thresholds, complications, monitoring, trauma and obstetric hemorrhage management for medical students and clinicians.
Choose Your Mode
How do you want to practice?
Study Mode
Learn at your own pace. Get instant feedback and detailed explanations after each question.
Start Studying
Exam Mode
Simulate real exam conditions. Timed questions, full scoring, and performance breakdown.
Take Exam
Strict Exam
Maximum difficulty. Full-screen, no backtracking, strict timing. For serious preparation.
Frequently Asked Questions
❓ What is blood transfusion?
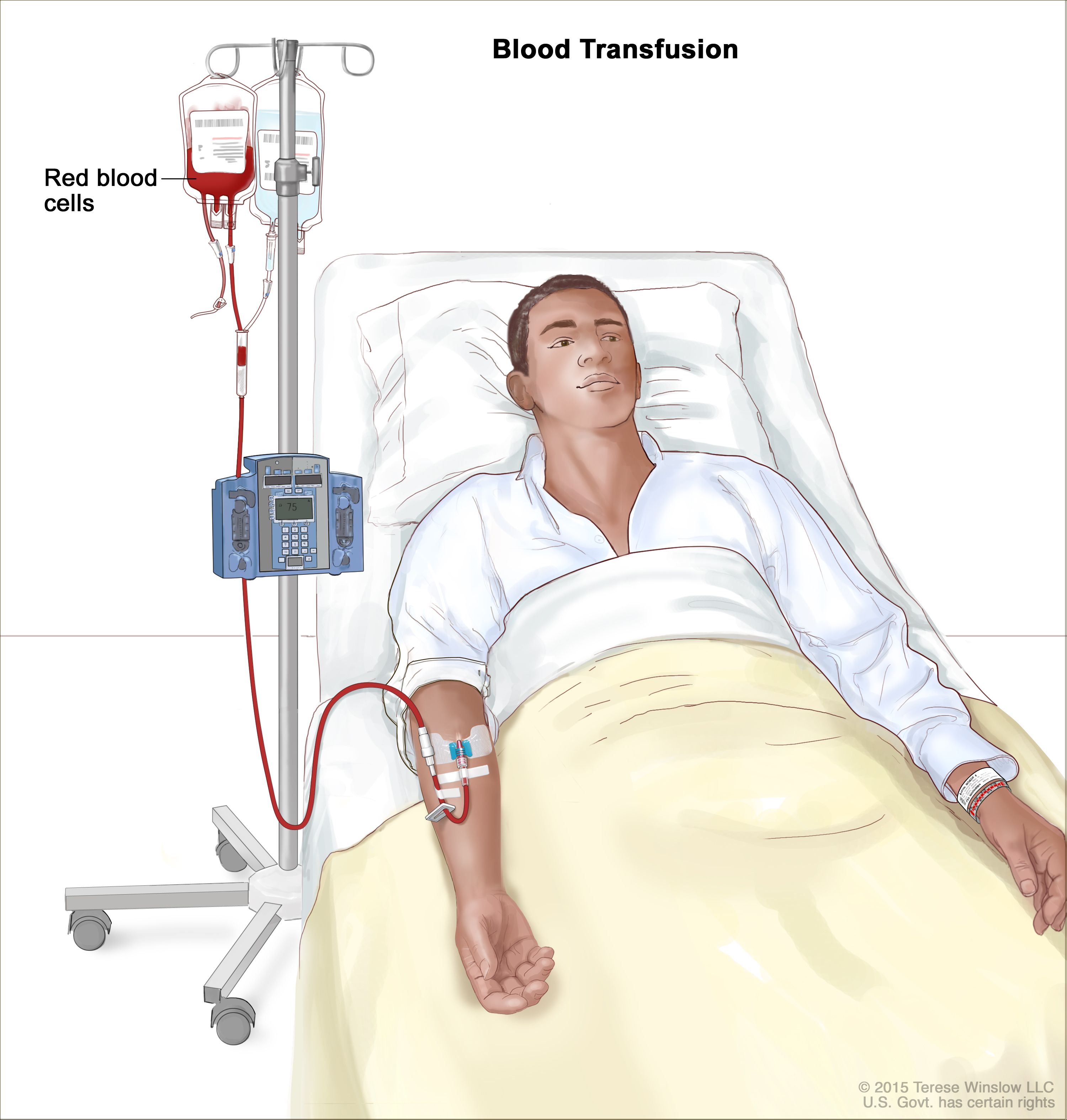
Blood transfusion is the intravenous administration of whole blood or specific blood components such as packed red blood cells, platelets, plasma, or cryoprecipitate to restore oxygen-carrying capacity, correct coagulopathy, or replace blood loss.
❓ What are the main indications for packed red blood cell transfusion?
PRBC transfusion is indicated in acute blood loss, symptomatic anemia, hemoglobin less than 7 g/dL in stable adults, hemoglobin less than 8 g/dL in patients with cardiovascular disease, and ongoing hemorrhagic shock.
❓ What is massive blood transfusion?
Massive blood transfusion is defined as transfusion of 10 or more units of PRBCs within 24 hours, 4 or more units within 1 hour with ongoing bleeding, or replacement of more than 50 percent of blood volume within 3 hours.
❓ When should a massive transfusion protocol be activated?
MTP should be activated in patients with life-threatening hemorrhage such as major trauma, postpartum hemorrhage, ruptured aneurysm, massive gastrointestinal bleeding, or uncontrolled surgical bleeding with hemodynamic instability.
❓ What is the recommended transfusion ratio in massive transfusion protocol?
The recommended ratio is 1:1:1 using packed red blood cells, fresh frozen plasma, and platelets to prevent dilutional coagulopathy and improve survival.
❓ Why is calcium supplementation required during massive transfusion?
Citrate used as an anticoagulant in stored blood binds ionized calcium, leading to hypocalcemia which can cause hypotension, arrhythmias, and reduced myocardial contractility.
❓ What are the most common complications of blood transfusion?
Common complications include febrile non-hemolytic transfusion reactions, allergic reactions, transfusion-associated circulatory overload, transfusion-related acute lung injury, hemolytic reactions, and transfusion-transmitted infections.
❓ How can TRALI be differentiated from TACO?
TRALI presents with acute hypoxemia, hypotension, and non-cardiogenic pulmonary edema, while TACO presents with hypertension, raised JVP, volume overload, elevated BNP, and improves with diuretics.
❓ What laboratory parameters should be monitored during massive transfusion?
Monitoring includes hemoglobin, platelet count, INR, PT, aPTT, fibrinogen levels, arterial blood gas, lactate, ionized calcium, electrolytes, and core body temperature.
❓ What is the role of tranexamic acid in massive transfusion?
Tranexamic acid reduces fibrinolysis and mortality when given early within 3 hours of trauma-related hemorrhage, usually as a 1 g IV bolus followed by 1 g infusion over 8 hours.
❓ When is platelet transfusion indicated?
Platelet transfusion is indicated when platelet count is below 10,000 per microliter prophylactically, below 20,000 with fever or sepsis, below 50,000 with active bleeding or surgery, and below 100,000 for neurosurgery.
❓ When should fresh frozen plasma be transfused?
FFP is indicated in active bleeding with INR greater than 1.5, massive transfusion, liver disease with bleeding, disseminated intravascular coagulation, and reversal of warfarin when PCC is unavailable.
❓ What is cryoprecipitate and when is it used?
Cryoprecipitate is rich in fibrinogen, factor VIII, factor XIII, and von Willebrand factor, and is used when fibrinogen levels fall below 150 to 200 mg/dL, especially in massive hemorrhage or DIC.
❓ What is the first step in managing a suspected acute hemolytic transfusion reaction?
The first step is to immediately stop the transfusion, maintain intravenous access with normal saline, assess the patient, and send blood and urine samples for hemolysis workup.
❓ When should massive transfusion protocol be stopped?
MTP should be discontinued once bleeding is controlled, the patient is hemodynamically stable, transfusion requirements decrease, and coagulation parameters begin to normalize.