💊 medicine
Mitral Regurgitation Detailed Management Guidelines Diagnosis and Treatment
Comprehensive guide on mitral regurgitation covering causes, pathophysiology, clinical features, echocardiographic diagnosis, acute and chronic management, medical therapy, surgical indications, mitral valve repair, replacement, and transcatheter options based on current cardiology guidelines.
Choose Your Mode
How do you want to practice?
Study Mode
Learn at your own pace. Get instant feedback and detailed explanations after each question.
Start Studying
Exam Mode
Simulate real exam conditions. Timed questions, full scoring, and performance breakdown.
Take Exam
Strict Exam
Maximum difficulty. Full-screen, no backtracking, strict timing. For serious preparation.
Frequently Asked Questions
❓ What is mitral regurgitation?
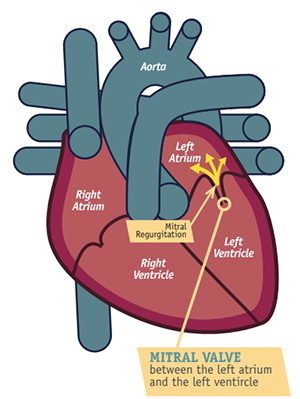
Mitral regurgitation is a valvular heart disease in which blood flows backward from the left ventricle into the left atrium during systole due to incomplete closure of the mitral valve.
❓ What are the main causes of mitral regurgitation?
Causes include mitral valve prolapse, rheumatic heart disease, infective endocarditis, papillary muscle rupture after myocardial infarction, dilated cardiomyopathy, and ischemic heart disease.
❓ What is the difference between acute and chronic mitral regurgitation?
Acute mitral regurgitation develops suddenly and causes pulmonary edema and shock, while chronic mitral regurgitation develops gradually with compensatory left atrial and ventricular dilation.
❓ What are the common symptoms of mitral regurgitation?
Symptoms include exertional dyspnea, fatigue, orthopnea, paroxysmal nocturnal dyspnea, palpitations due to atrial fibrillation, and hemoptysis in advanced disease.
❓ What is the characteristic murmur of mitral regurgitation?
Mitral regurgitation produces a holosystolic murmur best heard at the apex and radiating to the axilla, often accompanied by a soft first heart sound.
❓ Which investigation is the gold standard for diagnosing mitral regurgitation?
Echocardiography is the gold standard investigation, providing information about valve anatomy, severity of regurgitation, and left ventricular function.
❓ How is severe mitral regurgitation defined on echocardiography?
Severe mitral regurgitation is defined by effective regurgitant orifice area ≥0.40 cm², regurgitant volume ≥60 mL, or vena contracta width ≥0.7 cm.
❓ What are the indications for surgery in mitral regurgitation?
Indications include symptomatic severe mitral regurgitation, asymptomatic severe mitral regurgitation with left ventricular dysfunction, pulmonary hypertension, new-onset atrial fibrillation, or progressive ventricular dilation.
❓ Why is mitral valve repair preferred over replacement?
Mitral valve repair preserves left ventricular function, has lower operative mortality, avoids long-term anticoagulation, and provides better long-term survival.
❓ What is functional mitral regurgitation?
Functional mitral regurgitation occurs due to left ventricular dilation and remodeling with structurally normal mitral valve leaflets, commonly seen in ischemic or dilated cardiomyopathy.
❓ What role do medications play in mitral regurgitation?
Medications provide symptomatic relief and delay progression but do not correct the valve lesion; they include diuretics, ACE inhibitors, beta blockers, and anticoagulants when indicated.
❓ When is MitraClip therapy used in mitral regurgitation?
MitraClip is used in patients with severe symptomatic functional mitral regurgitation who remain symptomatic despite optimal medical therapy and are at high surgical risk.
❓ How does atrial fibrillation complicate mitral regurgitation?
Atrial fibrillation increases the risk of thromboembolism and worsens symptoms due to loss of atrial contribution to ventricular filling.
❓ Is mitral regurgitation tolerated during pregnancy?
Chronic mitral regurgitation with preserved left ventricular function is usually well tolerated during pregnancy due to reduced systemic vascular resistance.
❓ What is the most important prognostic factor in chronic mitral regurgitation?
Left ventricular systolic dysfunction is the most important predictor of poor prognosis and mortality in chronic mitral regurgitation.